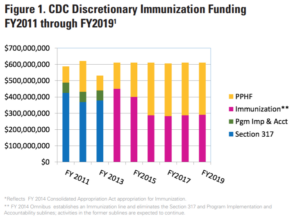
 The Prevention and Public Health Fund (PPHF) was created in 2010 as part of the Affordable Care Act. Originally intended to supplement core public health programs with increased investment in disease prevention and health promotion activities, the fund’s purpose evolved to support core immunization activities with more than half of immunization programmatic funding coming from PPHF starting in 2016.
The Prevention and Public Health Fund (PPHF) was created in 2010 as part of the Affordable Care Act. Originally intended to supplement core public health programs with increased investment in disease prevention and health promotion activities, the fund’s purpose evolved to support core immunization activities with more than half of immunization programmatic funding coming from PPHF starting in 2016.
Over $2 billion of PPHF funds have been invested in immunization, including over 700 million of PPHF for the 64 state, territorial, and local public health programs to support core activities in the nation’s existing immunization system.
PPHF makes up nearly half of all federal funding allocated to conduct immunization program activities.
Repeal of the Affordable Care Act without replacement of PPHF immunization funds would have immediate and catastrophic consequences:
Drop in Vaccination Rates
PPHF funding supports core immunization activities necessary to maintain high vaccination coverage levels, including staff and technology to track vaccination coverage and contain disease outbreaks. Vaccination rates cannot be sustained without strong immunization information systems (IIS) and experienced public health personnel to administer the Vaccines for Children program, train and educate providers and consumers, enforce school immunization requirements, respond to outbreaks, and conduct basic immunization program activities.
Job Loss
State and territorial immunization programs would experience a minimum 45% cut in program funding if PPHF were eliminated. This cut would result in massive layoffs to state and territorial health department personnel, impacting all aspects of the program from vaccine ordering to provider compliance.
Cuts to Local Health Programs
State and territorial immunization programs distribute PPHF funding directly to local health departments to conduct vaccination clinics, help respond to outbreaks, and work with local schools, WIC clinics, and other community partners to increase vaccination rates. A cut in PPHF would severely limit or end local immunization activities in most communities.
Disease Outbreaks
In 2016, cases of mumps more than tripled over 2015 levels. Outbreaks were reported in 7 states and cases of infection were reported in 46 states and the District of Columbia. Several university campuses experienced outbreaks involving hundreds of university students. In 2015 the U.S. experienced a serious outbreak of measles that affected states throughout the nation. Immunization program staff conduct thorough outbreak investigations, identify the source of diseases, prevent the spread of diseases by vaccinating contacts, and offer vaccines and education to affected communities. Without funding to support surveillance and vaccination, disease outbreaks would not be contained and the spread of disease would threaten all U.S. populations. The new threat of Zika virus as well as the continuing cases of mumps, measles, meningitis, hepatitis A, and pertussis demand continued support and funding for outbreak control and investigation.
Increased Risk to Newborn Babies
PPHF helps prevent the transmission of hepatitis B disease from mothers to babies. High risk babies are provided hepatitis B vaccine and treatment at birth to reduce the possibility of contracting the potentially fatal disease from their infected mothers. Without PPHF funds, immunization programs would not have resources to identify infants at risk for disease and provide the required treatment and vaccination to prevent transmission.
Elimination of Targeted Health Programs
PPHF supports special initiatives and programs that address the causes of low vaccination rates and reduce immunization disparities. For example, HPV vaccination coverage rates remain well below Healthy People 2020 goals. PPHF Funds targeted to HPV can help states improve HPV coverage rates to match existing rates for other adolescent vaccines, which would prevent around 12,000 cases of cervical cancer and approximately 4,000 deaths.
Loss of Critical Technology
Most immunization programs rely on PPHF to maintain and improve immunization information systems (IIS). These systems track vaccinations and share records with providers, parents and schools. They provide efficient vaccine ordering and accountability as well as identify areas of low vaccination and high risk for disease. PPHF is needed to sustain and enhance IIS functionality, continue to enroll providers and integrate IIS with electronic health records (EHRs).
Lack of Community Preparedness
PPHF is used as the cornerstone of public health emergency response to emerging threats such as Zika, the next influenza pandemic and natural and manmade disasters. Immunization programs continuously maintain, improve and test their response systems to prepare for potential threats.
Without PPHF, programs will not have the capacity to plan for and respond to emerging virus and disease threats.
